In this five-part series, Zaid Noorsumar examines gaps in news coverage of long-term care. Read Part 1 here.
PART II
In December 2003, the Toronto Star published a series of investigative stories on long-term care homes that exposed the brutal realities for residents and workers in Ontario. Spanning more than a week, the stories included the voices of residents, workers, family members, union leaders, home administrators and other industry insiders.
The reporting exposed drug errors, residents left unassisted until found by family members in their own feces, ants crawling on open sores on a person’s leg and other wretched tales that should never take place anywhere, much less in publicly funded care homes.
In response to the reportage, George Smitherman, the Ontario Liberal health minister, cried in front of cameras and promised a revolution in long-term care. As we now know all too well, no such transformation occurred.
That Toronto Star series shone a light on critical issues impacting long-term care but it also quoted Karen Sullivan, the CEO of the Ontario Long Term Care Association, as a “nursing home leader.”
Although the Star noted that the OLTCA mainly represents for-profit nursing homes, there was no critical examination of the impact of for-profit corporations on the sector.
Just the year before, in May 2002, the Ontario Health Coalition, an umbrella organization that represents patients, seniors and unions, released a research report, titled “Ownership Matters,” which detailed the damaging impact of the Progressive Conservative government (1995-2003) on the long-term care sector.
Perhaps the most important revelation in the report was the for-profit nursing home lobby’s re-regulation agenda that led to degradation of care in the entire sector. Even as the Harris-Eves Progressive Conservatives underfunded long-term care as part of austerity measures, the nursing home lobby extracted several concessions to ensure profits continued unabated.
The OHC’s report revealed that the OLTCA had successfully lobbied for the following policy changes since 1995:
- The removal of a minimum care standard (which had been instituted by the NDP in 1993 in response to pressure from health-care unions), which has yet to be restored as of 2021;
- The removal of a requirement to have a registered nurse on duty 24 hours a day (who could be replaced by less-trained and lower-paid staff);
- The increased allocation for “preferred beds” (for which nursing homes charge premium rates and which thereby contribute to profit margins);
- The removal of the requirement to return 50 per cent of surcharges for “preferred accommodation” back to the government (which could now be kept for expenses/profits);
- The removal of the requirement to submit staffing schedules annually to the ministry (thereby doing away with oversight).
In that same period, the Ontario PC government introduced a construction subsidy for building new homes regardless of ownership, which meant that for the first time, the province would fund the building of for-profit homes.
At the end of the home’s 25-30 year contract with the government to provide services (during which time they receive per diem funding for care plus the construction subsidy), the homes would be free to sell the real estate. (This policy continues today but is scarcely mentioned in the media, much less criticized for transfer of public funds to the private sector).
Over the last two decades, major Canadian media outlets have published a significant body of investigative journalism on long-term care, detailing instances of abuse and neglect.
But even as these stories questioned politicians about their lack of action, they ignored a key factor impacting effective change in the industry: the anti-public interest lobbying efforts of the businesses that own 58 per cent of Ontario’s long-term care homes and manage many non-profit and municipal homes.

This oversight, which I’ve observed through my analysis of coverage in mainstream news, appears not to be accidental. Traditional media’s own corporate structures and the imperative to maximize profits often means defaulting to normalizing private ownership and bears on its capacity to deliver a vital public service.
This trend has continued over the years predating the pandemic. Just prior to the 2018 election, the Toronto Star published an article featuring ideas from “health-care leaders” such as the executives of OLTCA and Home Care Ontario (both of them mainly represent for-profit firms, and neither were accurately identified).
Similarly, in 2017, a Toronto Star editorial named OLTCA among “advocates” for better care. More recently, in January 2021, the Star featured an opinion piece by Donna Duncan, the CEO of the OLTCA, calling for “decisive action” on long-term care.
In the 2003 series that exposed how short-staffing was leading to injuries, the Star quoted an OLTCA spokesperson who said she had told the ministry that funding for staffing was insufficient.
Although the Star’s stories did not investigate the impacts of operating nursing homes as a business, it did publish a few letters to the editor that highlighted this concern. One, for example, was penned by Natalie Mehra, the executive director of the Ontario Health Coalition, who pointed out that the Star’s business section had reported the month before that the major for-profit chain Extendicare’s “profits had soared” thanks in part to increased funding from the Ontario and Alberta governments.
Although the OHC has been a source for media outlets, it has scarcely been published on its criticism of private health-care corporations.
“I find it very frustrating because what bigger grassroots advocacy organization is there on health care in Ontario (besides us)?” said Mehra.
“There’s none. And to just ignore what we’re saying, and then report the voice of the for-profit industry uncritically means that the [media] reports are not accurate because they don’t give a full portrayal of what’s happening.”
In April 2002, the Toronto Star did feature an unusually in-depth investigative piece on the corporatization of the long-term care and retirement home sector.
The article exposed the precarious working conditions, as well as the broader structural issues that were hurting residents. It exposed the significant political donations to the ruling Ontario Progressive Conservatives, and the revolving door between industry and government.
But that turned out to be an aberration.
The fight for the minimum care standard
Based on feedback from advocates, the 2003 Star series offered a list of prescriptions to reform the sector. On top of that list was the restoration of a minimum care standard, which had been removed by the Progressive Conservatives in 1996.
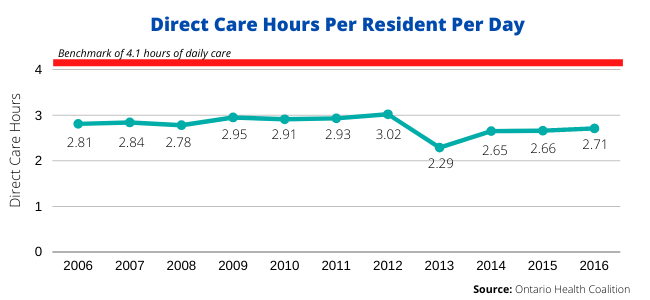
A minimum care standard refers to the (averaged) hands-on care that a resident receives on a daily basis by nurses and personal support workers, which naturally corresponds to staffing levels. In recent years, advocates have demanded a minimum standard of four hours of daily care per resident.
While campaigning for the October 2003 election, the Liberals had promised to restore the care standard. But Mehra, in her letter to the Star, noted that the health minister hadn’t committed to restoring it.
Without a care standard, homes are not accountable for how many staff work on the floor. Staffing levels are an important quality indicator in nursing homes, and research shows for-profit homes have lower staffing levels.
“The minister must ensure funding actually goes to resident care,” Mehra wrote. “He can do this by immediately establishing and enforcing minimum staffing standards in facilities. This is a simple regulatory change that all advocacy organizations for seniors agree upon.”
Mehra told J-Source that except for a brief period, the for-profit lobby has opposed a care standard — an angle that the mainstream media hasn’t shown interest in examining. (Between 2013 and 2015, Extendicare, one of the major for-profit firms, entered into an alliance with Unifor and SEIU to support a care standard).
In fact, through an ownership-agnostic point of view, the mainstream media continues to miss the story. Over the years, the Liberals delayed the implementation of a minimum care standard on one pretext or the other.
In 2007, the Ontario Health Coalition, unions and other groups relentlessly campaigned to have a minimum care standard included in the impending Long-Term Care Homes Act. In response, the Liberal government promised to include it in the legislation, before reneging on its promise.
The OLTCA and political lobbying
Among the glaring omissions in the media is any analysis of the influence of the for-profit lobby.
For instance, as I discovered while reporting for Rankandfile.ca,the OLTCA and the for-profit long-term care corporations donated over $650,000 to political parties in Ontario between 2007 and 2016 (corporate donations have been banned since). The OLTCA alone donated over $100,000.
“The Ontario Long Term Care Association has been powerful for a long time. They have a major say in what’s going on and how we understand the sector.”
Pat Armstrong
Over 95 per cent of the total donations went to the Ontario Liberals and the Progressive Conservatives, the two parties that have exclusively ruled Ontario since 1995 (the Health Coalition’s 2002 report catalogued political donations of close to half a million dollars between 1995 and 1999).
Corporations and their lobbyists donate to influence government policy, a dynamic explored in a 2001 CBC Marketplace report about the long-term care corporations that donated the most money appearing to win contracts to build new homes.
Moreover, corporations use PR lobbying firms to gain access to political officials. These firms hire ex-political staffers with insider knowledge and connections to elected officials.
As reported by Justin Panos for the Socialist Project and myself for Rankandfile.ca, the long-term care lobby has used over a dozen ex-staffers who previously worked for Liberals and Conservatives.
But aside from a few Toronto Star columns by Martin Regg Cohn that mentioned the OLTCA’s cash-for-access fundraisers with the Liberals in 2015-16 (and some more detailed reporting by Huffington Post’s Emma Paling during the pandemic), this continues to go unreported in most major publications.
The ex-political staffers-turned-lobbyists are no small fish. They include:
- Philip Dewan, former chief of staff to Liberal premier Dalton McGuinty (2003-2013);
- Bob Lopinsky, who was part of Kathleen Wynne’s 2014 election campaign and also involved in the McGuinty administration;
- John Duffy, the advisor to former Liberal prime minister Paul Martin.
Christina Bisanz was an Ontario Liberal candidate in the 2007 and 2011 elections. Between 2009 and 2011, she was also the CEO of the OLTCA.
While her affiliation with the OLTCA was mentioned as a biographical detail in an election results story, there tends to be no analysis of how conveniently political figures move between industry and government, and how such conflicts of interest impact policy making in our political system.
On the Conservative side, similarly prominent personnel have registered as lobbyists for private long-term care interests, even during the pandemic. The current CEO of OLTCA, Donna Duncan, was previously a senior advisor to John Tory in 2006-07, when he was the leader of the Progressive Conservatives in Ontario.
Until the pandemic, the media also did not speak about the fact that ex-Progressive Conservative premiers Mike Harris and Bill Davis sit on the boards of two LTC and retirement companies, Chartwell and Revera, respectively.
Despite these affiliations and details being available in the public domain, news organizations committed to investigative journalism have failed to highlight these problematic alliances.
Unfortunately, most mainstream media reports do not even inform their audiences about the nature of the OLTCA. It is often presented as an “umbrella group” that represents all types of nursing homes, including non-profit and municipal ones. However, 10 of the 12 positions on the OLTCA board are occupied by representatives of the for-profit industry.

According to my analysis of 201 news reports in six major outlets, out of the 23 times OLTCA was quoted in mainstream news in 2017-19, it was accurately depicted (as mainly representing for-profit homes) only five times. This trend continues during the pandemic.
Profiteers as advocates
In February 2019, the CBC’s investigative program Marketplace ran an episode Crying Out for Care, which delved into the perpetual neglect of residents in Canada’s long-term care homes, focusing mainly on Ontario. A recurrent theme during the show was the lack of staffing in these homes which led to resident abuse. Multiple times during the show, advocates spoke about the need for a staffing standard.
Towards the end of the show, Candace Chartier, then CEO of the OLTCA, said that homes needed more staff, elaborating that the association was calling for $100 million in additional government funding annually over the next four years.
This was an extraordinary claim considering that the staffing budget in long-term care homes was about $2.8 billion at the time. Another $100 million was a paltry sum.
In contrast, a June 2020 Centre for Policy Alternatives report estimated that adhering to the staffing levels recommended by experts would cost $1.6 billion (the Ontario Health Coalition had previously estimated the cost at $1.2 billion).
So why was the OLTCA asking for minimal funding at a time when long-term care homes were in crisis? The OLTCA declined J-Source’s request for an interview, suggested we send questions via email, and did not respond to subsequent emails. (Crestview Strategy’s Max Stern, who was previously involved in the federal Liberals’ 2015 election campaign, answered on the OLTCA’s behalf but did not respond to a number of specific questions asked.)
Unfortunately, viewers of the Marketplace investigation did not hear answers from the OLTCA to questions such as:
- Given there is legislation (Time to Care Act) for a staffing standard in the provincial parliament, why does the OLTCA oppose it?
- Why did OLTCA tell the Ottawa Citizen just over a year ago that the sector wasn’t in trouble and that “good news stories don’t hit the papers”?
- Why did its members continue to earn profits while residents languished in soiled diapers, died from preventable bed sores and assaulted overburdened staff who couldn’t meet their care needs?
Just days before the Marketplace episode aired, the Ontario Health Coalition released a thoroughly researched report titled Situation Critical. The report was superficially covered as most media outlets republished a variation of a Canadian Press article that was just over 500 words.
In response to the report’s recommendation that the government institute a minimum care standard, the Canadian Press reached out to the OLTCA. Chartier, the OLTCA’s spokesperson at the time, said that such a standard was a “cookie cutter approach” since not every person needs that level of care.
That statement, which ran unchallenged in the business press, is described as “specious” by Pat Armstrong, the distinguished research professor of sociology at York University, who has been studying the sector for decades.
“There are a number of different ways you could do the standard,” she says. “What the unions are calling for is the four hours of direct nursing care – you can distribute that any way you want. It isn’t a cookie cutter approach.”
Corporatization of long-term care research
In its 2018 and 2019 annual reports, the OLTCA made two extraordinary claims:
- Long-term care homes had made “great strides” in improving the quality of care over a five-year period from 2012-2016;
- Based on its assessment, there wasn’t a significant quality difference in homes based on ownership, a claim which contradicts a whole body of academic research carried out over decades.
But according to Armstrong’s comments in a Rankandfile.ca article I wrote in 2019, the OLTCA uses questionable metrics to arrive at these conclusions.
In its 2019 report, the OLTCA said it developed this assessment tool in partnership with the University of Toronto. But Nancy Cooper, a professor at the university’s Dalla Lana School of Public Health who was involved in this research, is also an OLTCA director. The OLTCA did not disclose that conflict of interest in its report.
Corporate influence on academic research, particularly on matters of public health, should be a grave concern. Yet there is no reporting on these issues so vital to a democratic society.
Kevin Skerret, a researcher for the Canadan Union of Public Employees, has tweeted about the corporate interests in cahoots with Ryerson University’s National Institute on Ageing. Specifically he highlights how the NIA’s advisory board includes people who represent for-profit homes.
The NIA has produced important work, and opinion pieces in mainstream media authored by its researchers and in the run-up to the 2019 federal election raised many important concerns regarding access to care, unsustainable burden on family caregivers and the predominance of women and immigrants in the sector (all of which are underreported or missing from regular reportage).
These are all components of the broader trend of privatization of care (which will be addressed in Part 3 of this series).
However, NIA’s corporate-sponsored research reports ignore the profit motive in the sector. Recently, Michael Nicin, NIA’s executive director, downplayed the impact of ownership on the quality of care.
“It is not clear to me that one class of ownership structure is doing noticeably better than any other,” he said, in an interview with the Financial Post.
Similarly, the Research Institute for Aging at the University of Waterloo is backed by Schlegel, the family-owned business empire that includes 19 long-term care and retirement homes in Ontario as well as Homewood Health Inc. (fun fact: Jagoda Pike, the former publisher of the Toronto Star, is the CEO of Homewood Health).
Since May 2020, the Star in particular has done some rigorous investigative journalism about the poorer quality in for-profit long-term care homes during the pandemic.
And yet, in November, the editorial board put the onus of responsibility for systemic failures on the provincial government. It wrote that if governments did regular inspections, and set standards, then “concern about for-profit models of care would lessen. The real problem is that government — not just this one but others before it, too — have never been particularly good at ensuring either of those things.”
This analysis ignores not just the inherent flaw of the profit motive, but is also oblivious to how corporate power impacts the government’s decision-making (which leads to reduced taxation on corporations and wealthy, less revenue for public services, corruption of academia and research, and stagnant wages for Canadians. It also, of course, ignores the long-term care lobby’s influence on the government.
Refusal to challenge power
The quality of reporting on long-term care has long fallen short of good, careful and accurate journalism. Some stories about this sector do win reporters journalism awards (some of which are backed by corporations) not just for exposing problems but for affecting policy changes.
But as explained in the academic paper, “It’s a Scandal,” media exposés on nursing homes have led to governments in the global North instituting more regulations, often to the detriment of better care. Unfortunately, they do not address structural changes.
Regulations around ownership, funding and staffing are critical to better care in long-term care homes, said Armstrong.
“The regulation tends to be focused on the staff and not on the owners and instead of on things like minimum staffing levels,” Armstrong says. “Why don’t we have that?”
I’d say that governments reluctant to challenge corporate power (often due to their own ties to business) tend to regulate in a particular way.
But policy changes don’t happen for the sake of it. Mike Harris did not simply decide that the long-term care sector needed to be re-regulated. The government was reacting to the pressure exerted by the nursing home lobby. To exclude that information, is quite simply, a failure of accurate and responsible journalism.
And although one can blame individual journalists (see Part 5), the refusal to challenge power is actually a systemic issue, considering that media organizations are corporate entities. To paraphrase the American academic and author, Michael Parenti: the media is corporate Canada.